The Role of Radiation in Advancing Medical Science- Few scientific discoveries have been met with such a mixture of wonder, fear, and transformative potential as radiation. When Wilhelm Röntgen stumbled upon mysterious rays in 1895, he couldn’t have imagined that his accidental discovery would fundamentally reshape medicine forever. Today, radiation stands as one of healthcare’s most powerful tools, simultaneously seeing inside our bodies and fighting our deadliest diseases.
A Serendipitous Revolution
The story begins on November 8, 1895, in Röntgen’s laboratory in Würzburg, Germany. While experimenting with cathode ray tubes, he noticed something peculiar: a fluorescent screen across the room glowed even though his tube was covered in black cardboard. He had discovered invisible rays that could penetrate solid matter—rays he called “X-rays” because their nature was unknown.
Within weeks, Röntgen produced the image that would change everything: a ghostly photograph of his wife’s hand, showing bones with her wedding ring floating eerily around one finger. The medical implications were immediately obvious. For the first time in human history, doctors could see inside the living body without cutting it open.
The medical community embraced X-rays with remarkable speed. By 1896—just months after Röntgen’s announcement—hospitals across Europe and America were using X-ray machines to locate bullets, diagnose fractures, and guide surgical procedures. What had taken surgery and guesswork could now be accomplished with a simple photograph.
The Double-Edged Sword Emerges
The early enthusiasm for X-rays came with a cost that nobody initially understood. Pioneer radiologists worked without protection, repeatedly exposing themselves to radiation. Some suffered severe burns, lost fingers or hands, and developed cancers. Thomas Edison’s assistant, Clarence Dally, became one of radiation’s first martyrs, dying in 1904 from radiation-induced cancer after extensive X-ray experiments.
These tragedies sparked a crucial realization: radiation demanded respect and careful handling. Scientists began studying radiation’s biological effects, leading to the field of radiation biology. Understanding both radiation’s harmful and therapeutic properties became paramount, ultimately making modern radiation medicine safer and more effective.
Paradoxically, the same properties that made radiation dangerous also made it medically valuable. If radiation could damage healthy cells, perhaps it could selectively destroy diseased ones.
Cancer’s Formidable Opponent
In 1896, just a year after X-rays were discovered, medical student Emil Grubbe in Chicago attempted one of the first radiation treatments for breast cancer. While that early attempt showed limited success, it opened a door to what would become radiation oncology—one of medicine’s primary weapons against cancer.
The early twentieth century saw rapid development in radiation therapy techniques. Marie Curie’s discovery of radium provided a powerful new radiation source. Doctors began inserting radioactive materials directly into tumors, a technique called brachytherapy that’s still used today in more refined forms.
Modern radiation therapy bears little resemblance to these crude beginnings. Today’s techniques use precisely targeted beams controlled by sophisticated computers. Intensity-Modulated Radiation Therapy (IMRT) can sculpt radiation doses to match a tumor’s exact three-dimensional shape, sparing surrounding healthy tissue. Stereotactic radiosurgery delivers incredibly precise, high-dose radiation to brain tumors without making a single incision.
Proton therapy represents the cutting edge, using accelerated protons instead of X-rays. These particles deposit most of their energy precisely at the tumor site, minimizing damage to tissue beyond the target—particularly valuable when treating childhood cancers or tumors near critical structures.
Diagnostic Imaging’s Quantum Leap
While X-rays revolutionized medicine, they were just the beginning. The mid-twentieth century brought an explosion of radiation-based imaging technologies that transformed diagnosis from educated guesswork into precise science.
The 1970s introduced Computed Tomography (CT) scanning, which combines multiple X-ray images taken from different angles to create detailed cross-sectional views of the body. Suddenly, doctors could see soft tissues, organs, and complex anatomical structures with unprecedented clarity. A CT scan can reveal internal bleeding in minutes, diagnose appendicitis without surgery, and detect tumors at treatable stages.
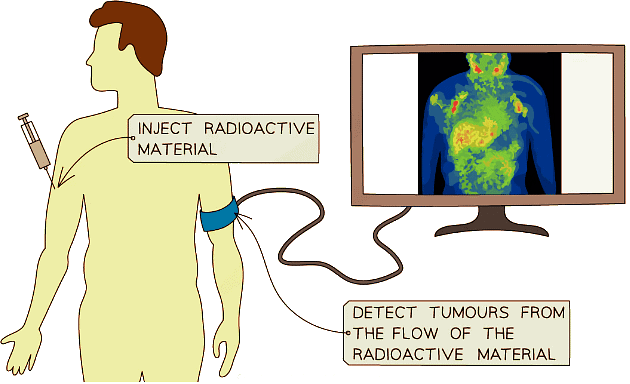
Positron Emission Tomography (PET) scanning took a different approach, using radioactive tracers to visualize metabolic processes in real-time. Cancer cells, which consume more glucose than normal cells, light up on PET scans like beacons. This technology revolutionized cancer staging, treatment planning, and monitoring, allowing doctors to see not just where tumors are, but how active they are.
Single-Photon Emission Computed Tomography (SPECT) imaging provides detailed information about blood flow and organ function. Cardiologists use it to assess heart muscle damage, neurologists to study brain activity, and oncologists to evaluate bone metastases.
Nuclear Medicine’s Targeted Approach
Nuclear medicine represents a sophisticated marriage of radiation physics, chemistry, and biology. Rather than beaming radiation from outside, nuclear medicine introduces radioactive substances into the body to diagnose or treat disease from within.
Radioactive iodine therapy for thyroid conditions exemplifies nuclear medicine’s elegance. The thyroid naturally concentrates iodine, so when patients ingest radioactive iodine-131, it accumulates specifically in thyroid tissue. This allows precise treatment of hyperthyroidism and thyroid cancer while sparing other organs—the ultimate targeted therapy.
Radiopharmaceuticals continue evolving. Lutetium-177 PSMA therapy for prostate cancer binds to a protein found on prostate cancer cells, delivering radiation directly to tumors throughout the body. This represents a paradigm shift: instead of shooting radiation at cancer from outside, we’re using the body’s own biological processes to deliver treatment with molecular precision.
Safety, Ethics, and the ALARA Principle
Modern radiation medicine operates under the ALARA principle: As Low As Reasonably Achievable. Every radiation exposure must be justified by medical benefit, optimized to minimize dose, and carefully limited to protect patients and healthcare workers.
Contemporary imaging equipment uses a fraction of the radiation dose required by early machines. Digital X-rays need less radiation than film, and advanced CT protocols adjust dose based on patient size and clinical indication. Lead shielding, distance, and time limits protect radiology staff, while sophisticated monitoring ensures no one receives excessive exposure.
The benefits vastly outweigh the risks when radiation is used appropriately. A chest X-ray delivers less radiation than a cross-country flight, while the information it provides can be life-saving. The key lies in using radiation judiciously—only when its diagnostic or therapeutic value justifies the minimal risk.
The Future Glows Bright
Radiation medicine continues evolving at a breathtaking pace. Artificial intelligence now helps radiologists detect subtle abnormalities in imaging studies, improving early cancer detection rates. Flash radiotherapy delivers ultra-high dose rates in milliseconds, potentially reducing side effects while maintaining tumor control.
Theranostics—combining diagnostic imaging and targeted therapy using the same radioactive molecule—represents medicine’s future. Doctors can first image where a radiopharmaceutical concentrates, then use a therapeutic version to deliver treatment to exactly those locations.
Researchers are developing “smart” radiopharmaceuticals that activate only in specific conditions, like the low-oxygen environment inside solid tumors. Others are exploring ways to combine radiation with immunotherapy, using radiation not just to destroy cancer cells but to train the immune system to recognize and attack cancer throughout the body.
A Legacy of Light and Hope
From Röntgen’s mysterious rays to today’s precision radiation medicine, this journey reflects humanity’s ability to transform a potentially dangerous phenomenon into a healing force. Radiation has given us eyes to see inside the body, weapons to fight cancer, and tools to understand biological processes at the molecular level.
Every year, millions of people benefit from radiation-based diagnosis or treatment. Cancers that were once death sentences are now curable. Internal injuries are diagnosed in minutes rather than through exploratory surgery. Thyroid diseases are managed with a simple pill rather than risky operations.
The story of radiation in medicine reminds us that scientific progress often comes from unexpected places, requires courage to pursue, and demands wisdom to use responsibly. As technology advances and our understanding deepens, radiation will undoubtedly continue playing a central role in medicine’s ongoing mission: to heal, to cure, and to extend the quality and length of human life.